MIPS Reporting for Behavioral Health in 2019
A Quick-Reference Guide for MIPS Compliance
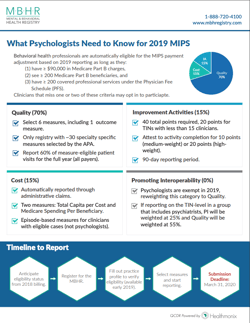
The Merit-based Incentive Payment System (MIPS) determines quality and efficiency of care through four performance categories: Quality, Promoting Interoperability, Improvement Activities, and Cost. Performance in these four categories during the 2019 calendar year will aggregate into a final score used to determine a payment adjustment for a MIPS-eligible clinician or group in the 2021 payment year.
